When working with children in speech and feeding therapy, it is important to recognize when something medical may be impacting progress. Tonsillitis is one of those conditions. While speech language pathologists do not diagnose tonsillitis, we are often the first to notice red flags during sessions. Parents may report symptoms like sore throat, fever, pain with swallowing, food refusal, drooling, bad breath, or changes in voice quality such as a muffled or hot potato voice. Clinically, you might observe enlarged or reddened tonsils, white patches, swollen glands, or a child who appears fatigued and avoids swallowing. These symptoms can significantly affect feeding and communication, leading to reduced oral intake, texture aversion, gagging, mouth breathing, hyponasal speech, and even decreased attention due to poor sleep.
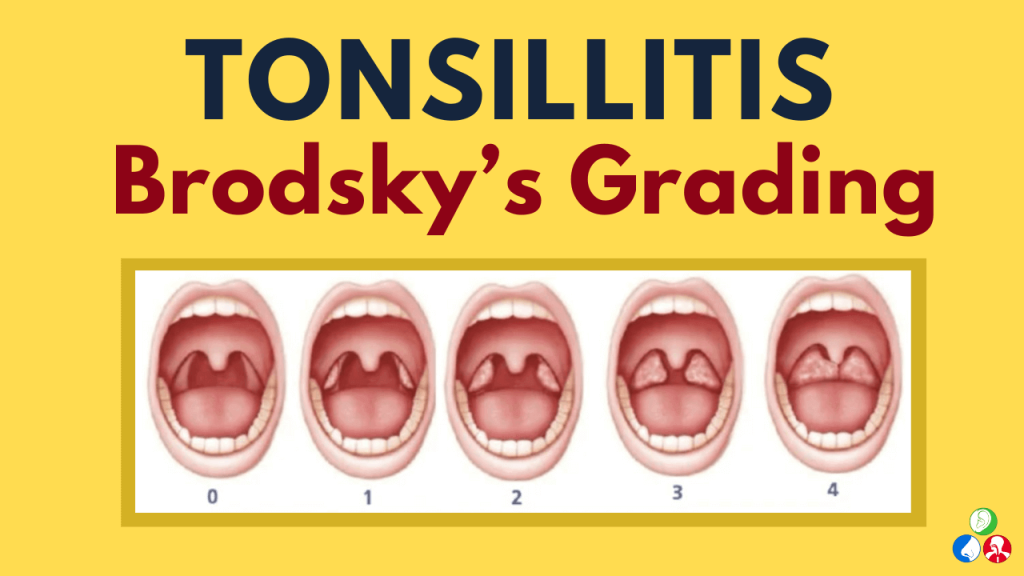
Tonsil size is commonly described using a scale from 0 to 4, which helps give context to what you are seeing. Grade 0 means the tonsils have been removed. Grade 1 tonsils sit within the tonsillar pillars and are often barely visible. Grade 2 tonsils extend just outside the pillars and are still considered within normal limits. Grade 3 tonsils are enlarged and take up more space in the throat, often approaching the midline and potentially impacting airflow or swallowing. Grade 4 tonsils are significantly enlarged and may touch at the midline, sometimes referred to as kissing tonsils, and are much more likely to interfere with breathing, sleep, voice quality, and feeding.
Because these symptoms can interfere with both feeding and speech outcomes, timely referral is key. If a child presents with difficulty breathing, excessive drooling, inability to swallow, high fever, dehydration, or significant asymmetry in tonsil size, immediate medical evaluation is warranted. Even in less urgent cases, recurring throat infections or chronic snoring and mouth breathing should prompt a referral to a pediatrician or ENT. As speech language pathologists, our role is to support the child holistically by recognizing when progress is being impacted by underlying medical factors and ensuring families are guided toward appropriate care so therapy can be as effective as possible.ropriate care so therapy can be as effective as possible.
Warmly,
The Speech in the City Team